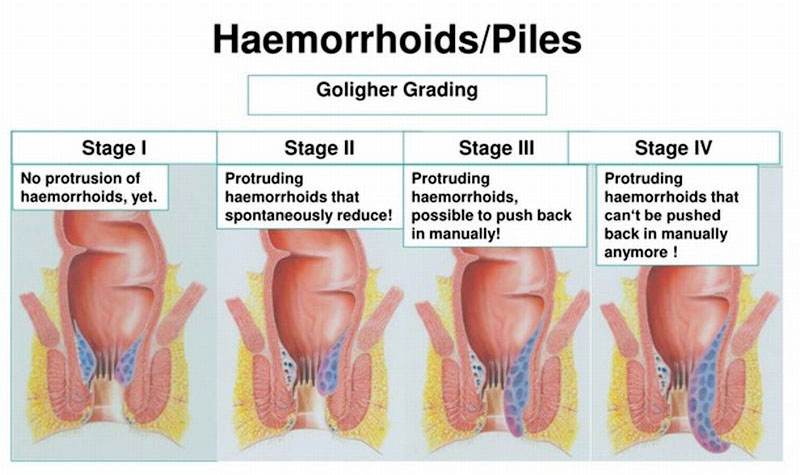
The commonly accepted definition of anal fissure is: “A linear ulcer of the anoderm, distal to the dentate line, generally located in the posterior midline”. Only a carefully selected group of patients, without anal hypertonia, could benefit from anoplasty. The risk of incontinence after this procedure seems to have been overemphasized in the past. Nonresponding patients should undergo lateral internal sphincterotomy. Use of 0.4% glyceryl trinitrate in standardized fashion seems to have the best results despite a higher percentage of headache, while the use of botulinum toxin had inconsistent results. While there is little chance of a cure with conservative behavioral therapy, medical treatment with calcium channel blockers, diltiazem and nifepidine or glyceryl trinitrate, had a considerable success rate ranging from 50 to 90%. This review is aimed at identifying the best treatment option drawing on evidence-based medicine and on the expert advice of 6 colorectal surgeons with extensive experience in this field in order to produce an Italian position statement for anal fissures. Despite some systematic reviews and an American position statement, there is ongoing debate about the best treatment for anal fissure. In the last decades, the understanding of its pathophysiology has led to a progressive reduction of invasive and potentially invalidating treatments in favor of conservative treatment based on anal sphincter muscle relaxation. Its treatment has long been discussed and several different therapeutic options have been proposed. 
Longer internal anal sphincter division (to the dentate line, as opposed to the fissure apex only) may be more effective at reducing anal fissure.Anal fissure is one of the most common and painful proctologic diseases. Open partial lateral internal anal sphincterotomy may be equivalent to closed partial internal anal sphincterotomy in fissure healing. 
We do not know whether internal anal sphincterotomy is better or worse than anal advancement flap in improving fissure healing. We do not know whether anal dilation is more effective than topical nitroglycerin at reducing the proportion of persons with anal fissure. One small randomized controlled trial found limited evidence that controlled anal dilation may be equivalent to sphincterotomy in fissure healing, with negligible incontinence risk. Internal anal sphincterotomy also increases fissure healing compared with digital anal stretch, and anal stretch is more likely to cause flatus incontinence. It improves fissure healing compared with treatment with nitric oxide donors (topical nitroglycerin, topical isosorbide dinitrate), botulinum A toxin–hemagglutinin complex, and calcium channel blockers (nifedipine, diltiazem). 
Internal anal sphincterotomy is more effective than medical therapy for chronic anal fissure in adults. The cause is not fully understood, but low intake of dietary fiber may be a risk factor.Ĭhronic fissures typically have a cyclical history of intermittent healing and recurrence, but about 35% will eventually heal, at least temporarily, without intervention.Ītypical features, such as multiple, large, or irregular fissures, or those not in the midline, may indicate underlying malignancy, sexually transmitted infections, inflammatory bowel disease, or trauma. Anal fissures are a common cause of anal pain during and for one to two hours after defecation.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
